Mixed use refers to a mix of land uses in close proximity. It is applicable at scales ranging from a single site to a full district. There are four types of mixed use: vertical mixed use, mixed use districts, mixed use developments, and urban design guidelines / form-based codes.
Why is this important to your community?
Residents in the outer counties of the CONNECT Region have higher rates of hospitalization for chronic disease and have access to fewer health resources and facilities (see CONNECT Public Health Work Group report). All of the counties within the CONNECT region, with the exception of Mecklenburg County, have a lower concentration of physicians and includes 14 medically underserved areas. Counties not adjacent to the Charlotte urban area—Stanly, Anson, Union, and Chester–have hospital discharge rates 20% higher (i.e. worse) than the state average, higher unemployment rates, lower household income, higher poverty levels, and lower rates of educational attainment.
Skip directly to
How Does It Work?
Resources
Using the Tool
Partners
Where Has It Worked?
Where is it appropriate to use?
What priorities does it address?
What other tools are related?
How does it work?
According to the American Telemedicine Association, there are currently about 200 telemedicine networks in the US, with over half of hospitals using some form of telemedicine. Telemedicine is considered a safe and cost-effective way to expand the delivery of healthcare, particularly access to specialists, when guided by technical standards and clinical practice guidelines.
Resources
Ready to get started?
Using the Tool
- Meet with the local health department, medical society(ies,) and representatives from area hospitals, clinics and advocacy groups to discuss options for meeting the needs of populations lacking access to health care facilities, and/or populations needing more specialized care than is typically available in the community, county, or region. Is telemedicine an option?
- If the answer is yes, convene a working group including medical professionals, technology experts, local officials, and other partners to develop an appropriate delivery method for telemedicine in the region. Is it a pilot program headed by a large health care system, a smaller deployment of teleconferencing employed by one or more individual physicians, or some other technique?
- Provide support to implement the appropriate delivery method determined by the working group. This may take the form of providing loans or grants to extend broadband access or helping to remove regulatory barriers to telemedicine.
Partners
Where has it worked?
The Heart Success (HS) Transition Clinic at Carolinas Medical Center (CMC) Main and CMC NorthEast - Carolinas HealthCare System, North and South Carolina
About the Program
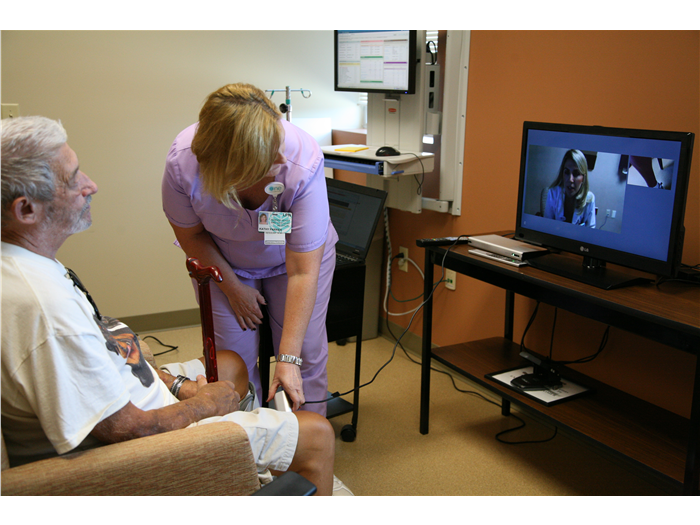
In an effort to address heart failure patients with high rates of hospitalization, Carolinas HealthCare System piloted the Heart Success Transition Clinic. Initially, the program had patients meet with a medical team at the clinic each week for the duration of the program. However, after seeing initial success, clinicians realized they were not reaching 25% of discharged patients. The primary reason was the long distance between the patients’ homes and the clinic locations. In 2013, the HT Clinic launched a virtual model of the original pilot program. Patients discharged from a regional health clinic meet virtually with the medical team using videoconferences while the team remotely monitors vital signs using a peripheral stethoscope.
Why it works
The virtual HT Clinic not only makes treatment accessible to remote patients cost effective and convenient, it also decreases repeat hospitalizations and helps patients understand and manage their own medical care. Over the course of the six month pilot, the program treated 60 patients in the virtual HT Clinic, and recorded an almost 8% decrease in readmission rates. In addition to a drop in readmission rates, the medical team noticed that patients reacted positively to the telemedicine appointments and began taking ownership of their own health and health outcomes.
http://denverncweekly.com/news/2013/9/6/2880/cmc-lincoln-launches-virtual-care-initiatives